The origin of Respecting Choices stems back to 1985 when its founder, Bud Hammes, had just started his career as a clinical ethicist at Gundersen Health System. He was struck by the frequency of moral distress experienced by both families and physicians faced with critical choices about treatments for patients who lacked decision-making capacity to participate in their healthcare decisions. What appeared striking to Hammes about these instances was that the patients were typically older, they had prolonged periods of worsening health, and there was ample opportunity of engaging the patients in planning. It wasn’t that patients were making the decision not to plan. Rather, there was nothing in the healthcare system that helped them to plan and health professionals had no training or workflows to make it happen.
Determined to address this issue, Hammes requested support to build an advance care planning (ACP) process/system in a dialysis unit that cared for 60 patients at the former Lutheran Hospital. In 1986-87, the “If I Only Knew…” program was designed, created, and implemented to provide a comprehensive, organized system of educating nurses to facilitate conversations with dialysis patients and families. The program equipped staff with standardized patient engagement materials, reliable documentation of ACP conversations, patient plans that addressed the most frequent decisions faced by dialysis patients, and education (for Emergency Room staff and physicians) to know where to locate this planning information and how to apply the plans to clinical decision making.
Within a few years, the prevalence of advance directive (AD) documents increased from one out of 60 people to 30 out of 60. But more importantly, during times of critical decisions, not only were well-developed plans available and clear, but family members were also engaged and satisfied with the new model of care. For this small population of dialysis patients, moral distress of both family as well has health professionals largely disappeared regarding decisions of whether to continue or discontinue life-sustaining treatment.
The next development was unexpected and dramatic. In the late 1980s and early 1990s, the leaders of the major health organizations in La Crosse, Wisconsin, were exploring ways that they could collaborate to improve the health of the community. Two of those leaders were part of the Gundersen Health System and were very familiar with the success of the planning process in the Lutheran Hospital dialysis unit. These leaders asked, “Why couldn’t we do this for the whole community?’’ They decided to try.
In 1990, they appointed a community task force, chaired by Bud Hammes, to develop a multi-faceted program to improve care through the creation and implementation of an ACP program. It was this program that came to be called Respecting Choices. The first Facilitator education was offered in 1993 in La Crosse, Wisconsin, and represented the final necessary piece of the implementation that included development of organizational policies on ACP, the development of patient engagement materials, the design of medical records systems, and the education of physicians.
Quality improvement principles guided the development and enhancement of this grassroots community program. Funding was secured to more rigorously evaluate the impact of the La Crosse Respecting Choices program. The first La Crosse Advance Directive Study (LADS I) commenced in 1995-96. This research studied all adult La Crosse County residents who died under the care of any health organization in La Crosse County (N=540). The findings showed that 85% of decedents had some type of written AD, 96% of these documents were found in the medical record of the treating health organization, and the preferences to forgo treatment in these documents were consistent with treatment decisions 98% of the time. When published in 1998, these findings created an interest in Respecting Choices from health organizations across the United States.
By 1999, the LADS I article was generating significant interest in the Respecting Choices program by health organizations from many parts of the United States. This new interest resulted in the Gundersen Lutheran Medical Foundation approving the creation of a new position to help revise the local Respecting Choices materials and to deliver these materials and education to a national audience. Linda Briggs’ experience as a critical care nurse specialist, clinical ethicist, and curriculum development specialist provided a strong background for the position of Associate Director of Respecting Choices. Briggs started on July 1, 1999, launching the international platform for Respecting Choices.
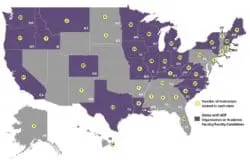
The first national Respecting Choices education occurred in La Crosse in Spring 2000. This was a 4-day course that provided Facilitator Certification (2 days); Design and Integration content (1 day); and Instructor Certification (1 day). Briggs and Hammes began the process of learning how to transfer the success of Respecting Choices in La Crosse, Wisconsin, to other places in the United States and beyond. The Respecting Choices program transferred to Australia in 2002, to health systems in Canada starting in 2004, to Germany for a research project in 2007, and to Singapore in 2009.
 Over subsequent years, Briggs and Hammes continued to evaluate the national curriculum materials and strategies to learn the most effective approaches to best assist health organizations and communities to be successful at creating person-centered, ACP systems. The evolution of Respecting Choices continues today and is made possible by the contributions, partnerships, and research of many individuals, organizations, and communities around the world. Based on these collaborations, Respecting Choices now offers an array of educational and consultation services that includes leadership engagements, onsite assessments, a physician curriculum, First Steps® ACP, Next Steps™ ACP, and Advanced Steps ACP implementation services that include a customized approach integrating the organization’s needs, resources, and goals.
Over subsequent years, Briggs and Hammes continued to evaluate the national curriculum materials and strategies to learn the most effective approaches to best assist health organizations and communities to be successful at creating person-centered, ACP systems. The evolution of Respecting Choices continues today and is made possible by the contributions, partnerships, and research of many individuals, organizations, and communities around the world. Based on these collaborations, Respecting Choices now offers an array of educational and consultation services that includes leadership engagements, onsite assessments, a physician curriculum, First Steps® ACP, Next Steps™ ACP, and Advanced Steps ACP implementation services that include a customized approach integrating the organization’s needs, resources, and goals.
Conducted in 2007-08, LADS II repeated the same methodology in the same population and health facilities as was used in LADS I. In this study, 400 consecutive adult deaths were reviewed from all settings of care in La Crosse County to see if the findings of LADS I were being maintained after 10 years. The results showed the prevalence of written AD increased to 90%, written directives were found in the decedents medical records 99% of the time, and preference for or against treatments were consistent with treatments 99% of the time.
To continue assisting health systems, organizations, and communities successfully develop person-centered care and sustain this culture, Gundersen Medical Foundation and Respecting Choices realized it needed a new platform for purposes of growth, improvement, and sustainability to meet its national and international mission. In January, 2017, Gundersen transferred the Respecting Choices program and team members to C-TAC Innovations, a new, independent, not-for-profit organization that is affiliated with the Coalition to Transform Advanced Care (C-TAC).
Expanding Reach and Access to Personalized Patient Decision Support and Advance Care Planning
The delivery of care has evolved since Respecting Choices’ inception, but the evidence-based foundation of its programs remains as relevant as ever. Embracing the principle of “freedom within a framework,” the Respecting Choices team adapted their implementation models to meet the unique needs of customers and their settings.
In this spirit of adapting to and growing with change, Respecting Choices joined WiserCare in September 2023. WiserCare is a pioneer in digital patient decision support and ACP experiences, with a focus on helping customers deliver personalized care, and proven results showing high patient, family, and provider satisfaction and positive impacts on the quality and value of care delivery. By joining WiserCare, Respecting Choices adopted another innovative strategy to help health systems, health plans, and communities provide ACP services more efficiently. The integrated organization continues to offer WiserCare’s portfolio of clinically integrated patient decision support modules, as well as Respecting Choices’ full-spectrum of best-in-class interprofessional training, implementation, and capacity building services.
The Respecting Choices program already has a long history of creating person-centered care through the implementation of effective ACP systems. This robust intervention shows clear signs of success and sustainability. Respecting Choices welcomes many new partners and collaborators to share in creating the next chapter of this history.

